
The Mystery of US Construction’s Declining Productivity
The sector’s slowdown is so great it represents a drag on the economy overall.
The Mystery of US Construction’s Declining Productivity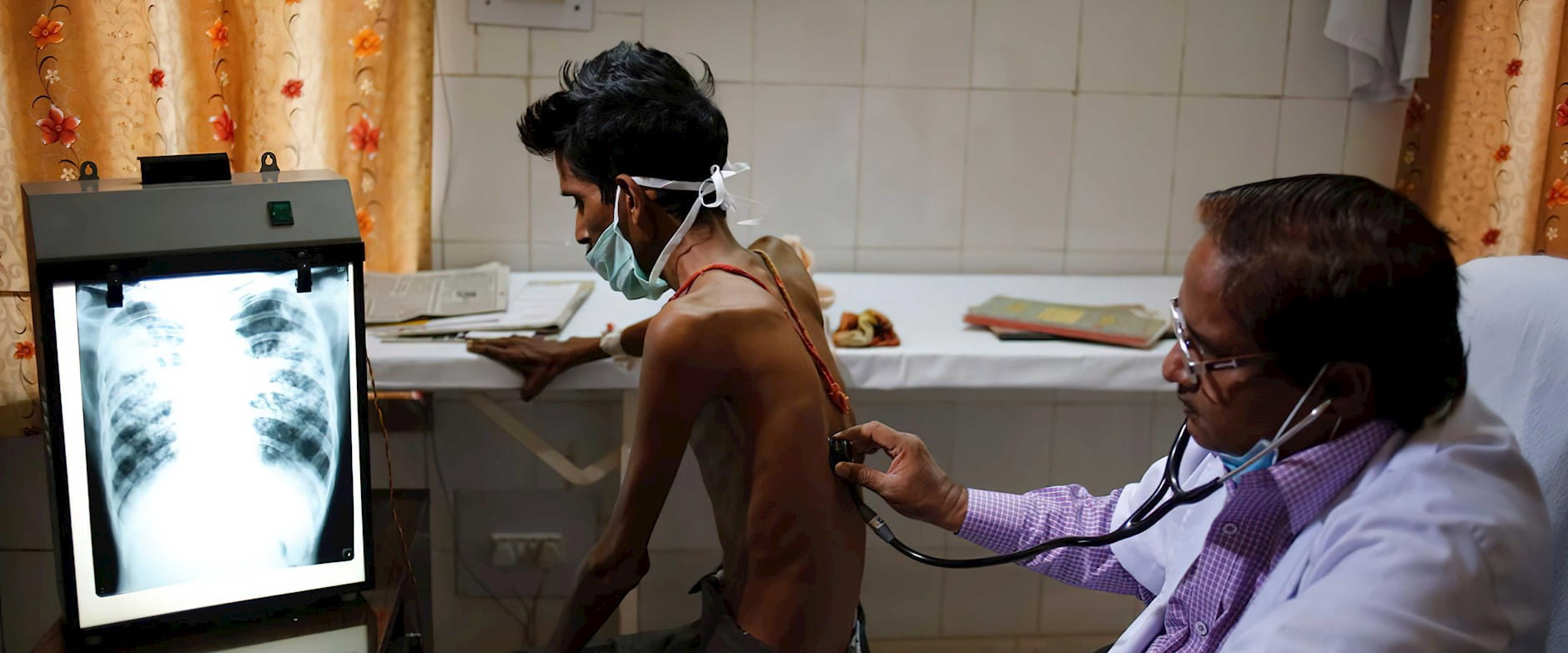
Associated Press
Tuberculosis is the world’s leading infectious cause of death, killing almost 1.7 million people worldwide in 2016. One of the biggest challenges of treating the highly contagious bacterial disease in developing countries is simply identifying patients.
But social networks can help, according to research by University of Maryland’s Jessica Goldberg, Johns Hopkins’s Mario Macis, and Chicago Booth’s Pradeep K. Chintagunta. In a study conducted in India, they find that patients already in treatment are more effective than health workers at persuading potential TB sufferers to get screened.
The research has significant implications for the treatment of TB and other communicable diseases in developing countries.
TB spreads from person to person through the air, typically attacking a person’s lungs and destroying tissue. It infects about 3 million new patients a year in India, where an estimated 40 percent of cases go unreported. But with antibiotics, TB can be treated and cured.
The researchers worked with Operation ASHA, a nongovernmental organization that runs TB treatment centers in 11 Indian states, to conduct a randomized controlled trial of peer-referral models at 122 treatment centers between March 2016 and October 2017. They had patients and health workers conduct outreach to suspected TB sufferers and experimented with offering economic incentives, which included making cash payments dependent on a subject’s test results.
The results suggest that coupling peer outreach and financial incentives can not only yield better results but also be cheaper.
Goldberg, Macis, and Chintagunta find that existing patients were “able and willing” to identify and bring in suspected TB patients for testing. The 3,176 patients in various treatment groups produced 222 new suspected patients, 176 of whom had symptoms and were sent for testing, and 36 of whom were diagnosed with the disease. Patients offered a financial incentive of 150 rupees, about $3, were more likely to make a referral than those who were only encouraged to do so. Offering higher payouts for referrals that resulted in a TB diagnosis did not have a significant effect compared with incentives or encouragement that did not include this condition.
Outreach by current patients resulted in more than twice as many potential patients being screened and tested than outreach by health workers. Peers, the researchers suggest, may be “more effective in conveying information about the benefits of treatment.” And peer outreach brought in patients who had fewer social connections, according to the researchers’ measure, than those identified by health workers.
The results suggest that coupling peer outreach and financial incentives can not only yield better results but also be cheaper. Identifying patients via peer referral cost 25–35 percent as much as identification via health-worker outreach.
“Because of the effectiveness of small financial incentives and the comparatively lower cost of time for current patients than health workers, incentivized peer outreach in TB detection is highly cost-effective,” the researchers write.
Jessica Goldberg, Mario Macis, and Pradeep K. Chintagunta, “Leveraging Patients’ Social Networks to Overcome Tuberculosis Underdetection: A Field Experiment in India,” Working paper, November 2018.

The sector’s slowdown is so great it represents a drag on the economy overall.
The Mystery of US Construction’s Declining Productivity
Susan Athey, chief economist at the US DOJ’s antitrust division, joins hosts Bethany McLean and Luigi Zingales to discuss new draft merger guidelines.
Capitalisn’t: The Most Important Guidelines You Didn’t Know About
Is inefficiency inherent in the matching of students and colleges?
How Colleges Can Make the Admissions Process Easier for Students, and ThemselvesYour Privacy
We want to demonstrate our commitment to your privacy. Please review Chicago Booth's privacy notice, which provides information explaining how and why we collect particular information when you visit our website.